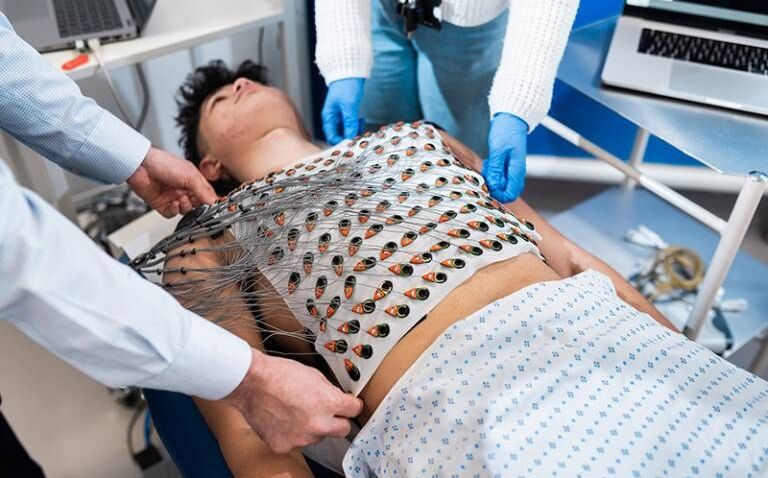
A new study led by researchers at University College London (UCL) highlights how cardiovascular magnetic resonance (CMR)-guided electrocardiographic imaging (ECGI) can be used to detect hypertrophic cardiomyopathy in subclinical cases.
Individuals carrying sarcomere gene mutations but with no detectable symptoms associated with hypertrophic cardiomyopathy (HCM) exhibited abnormal electrical patterns in the heart using a new electrocardiographic imaging (ECGI) vest.
The abnormalities were not detected on standard ECGs, and no structural changes were observed in the heart.
The findings are published in the Journal of the American College of Cardiology and could help clinicians identify abnormalities associated with HCM much earlier than is currently possible.
CMR-guided ECGI can create images of the heart showing its cardiac structural features and electrophysiological properties. The researchers wanted to determine whether ECGI using a reusable vest can identify early electrical abnormality in individuals with subclinical HCM who have a genetic predisposition (genotype [G]+) but do not yet show left ventricular hypertrophy (LVH−). They also examined how the electrophysiological substrate influenced the findings.
The researchers enrolled 211 participants (70 G+LVH−, 104 LVH+ (51 G+/53 G−), and 37 healthy volunteers) to a CMR-ECGI multicentre study. Local activation time (AT), corrected repolarisation time corrected activation-recovery interval, spatial gradients (GAT/GRTc), and signal fractionation were derived from 1,000 epicardial sites per participant. Maximal wall thickness and scar burden were derived from CMR. The researchers built a support vector machine to discriminate G+LVH− from HV and low-risk HCM from those with intermediate/high-risk score or nonsustained ventricular tachycardia.
The team found that the ECGI vest identified electrical abnormalities in a quarter of individuals with a gene mutation for whom no signs of disease were detected via either MRI or standard 12-lead ECG.
In participants with subclinical HCM, a significant prolongation of AT was observed, and the repolarisation phase was found to be more irregular. Approximately 23% of individuals with subclinical HCM had normal results on standard ECG tests.
Participants with overt HCM were found to have a more prolonged activation-recovery interval than those with subclinical HCM, and participants with thicker heart walls tended to have longer ATs.
Spatial conduction heterogeneity and fractionation of electrical signals were both correlated with the presence of scar tissue in the heart.
Individuals with both the genetic mutation associated with HCM (G+) and LVH+ showed more fragmentation of electrical signals in their heart compared to those who only had LVH+ but did not carry the genetic mutation (G-).
Lead author Dr George Joy, cardiology registrar and British Heart Foundation clinical research training fellow at the UCL Institute of Cardiovascular Science and Barts Heart Centre, said: ‘By finding subtle electrical abnormalities using our new technique, we are able to detect hypertrophic cardiomyopathy earlier. This is important as it means we can potentially act earlier, providing new treatment to slow the disease as well as fast-tracking individuals to clinical trials that have potential to stop the disease entirely.’
The researchers also applied a machine learning algorithm to the results of 12 markers from the ECGI vest. They found they could correctly distinguish between individuals with subclinical HCM patients and healthy volunteers 80% of the time. The algorithm also identified patients at high risk of sudden cardiac death 82% of the time.
Dr Joy added: ‘Next steps of the research include repeating these results in a larger group of patients and following individuals over time to see how these early electrical changes affect the risk of life-threatening heart rhythms later on.’
Last year, the team found that using two cutting edge heart scanning techniques to scan patients with hypertrophic cardiomyopathy enabled the identification of microstructural and microvascular disease changes that can serve as early-phenotype biomarkers for the condition.
Image courtesy of UCL Institute of Cardiovascular Science / James Tye.