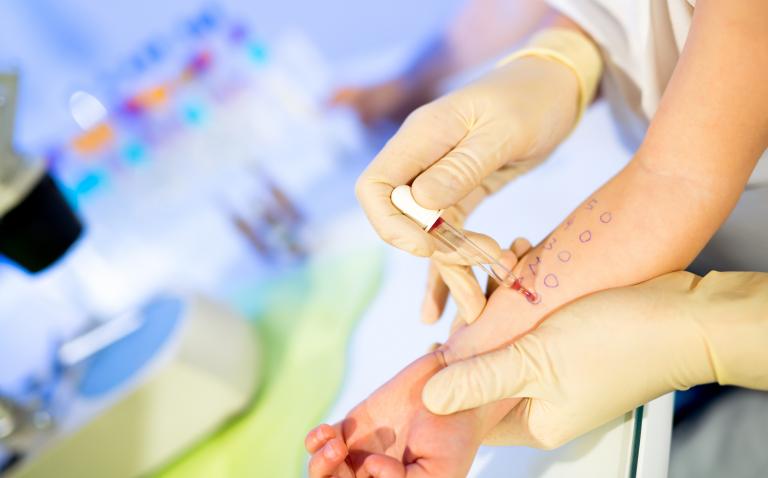
Individuals who suffer from allergic problems, such as rhinitis, bronchial asthma, food allergy or atopic dermatitis, are usually subjected to allergic skin tests to reveal the causative factors, to put prevention strategies in place, and to implement the most suitable therapy.
The prick test is helpful in the diagnosis of immediate hypersensitivity reactions (there are other types of reactions, defined as ‘delayed’, which occur mostly as contact dermatitis, and which require other types of test). The prick test is performed on an outpatient basis, in just a few minutes.
To perform the prick test, it is important that the patient has not taken anti-histamines by mouth (or injection) for at least 5-7 days (depending on the type of anti-histamine). In general, other therapies do not interfere with testing.
The prick test is carried out by placing a drop of an allergenic extract (food or inhalant type: pollen, derivative of dust mites or pets, etc.) on the patient’s skin. The skin of the area chosen for the test is usually the volar face of the forearm: and more precisely 5cm above the wrist and 3cm below the antecubital fossa. Subsequently, the allergist ‘pricks’ the skin underlying the allergenic drop with a sterile lancet (usually made of plastic or steel). It is necessary to use a different sterile lancet for each allergen, to avoid cross-contamination.
Allergenic molecules are then able to penetrate the superficial layers of the skin and come into contact with the IgE present on the surface of the mast cells. Once the puncture has been performed, the allergenic solution can be removed with a cotton, gauze or paper swab. After about 15 minutes, the skin is examined to assess any positive reactions to one or more allergens, which appear as rounded and raised wheals, several millimetres in diameter, that are itchy and surrounded by erythema. The wheals appear in all respects similar to ‘mosquito bites’.
For better diagnostic accuracy, positive and negative controls in addition to the selected allergens are performed. The positive control, with histamine, is used to assess skin reactivity and may be negative (non-reactive) in cases of anti-histamine therapy or in other cases of skin anergy; in these situations, the result of the prick test is not reliable. The negative control, which is carried out with saline solution or glycerin, is used to document any cutaneous hyper-reactivity: even in this case, if it is positive, the test result is not reliable.
The prick test can be performed at any age, but it is considered not to be reproducible and more difficult to interpret before the age of three years.
The prick test can be performed at any time of the year, even for seasonal allergies, subject to the necessary suspension of any therapies with antihistamines.