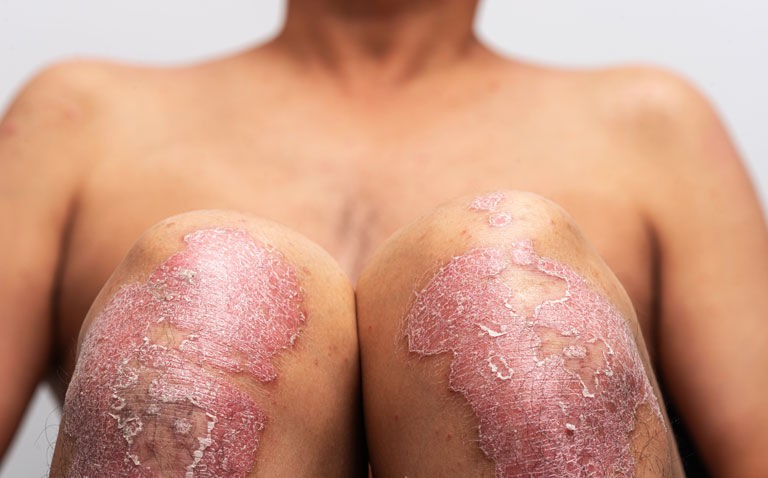
A randomised trial has found that oral vitamin D supplementation makes no difference to disease severity in patients with psoriasis
Norwegian researchers have found that oral vitamin D supplementation given throughout the winter months to patients with psoriasis, despite increasing serum levels of the vitamin, does not lead to an improvement in disease severity.
One aspect of treatment for psoriasis involves the use of topical vitamin D although whether oral vitamin D is also an effective form of therapy remains to be clarified. One randomised trial concluded that oral vitamin D2 increased both serum vitamin D levels and disease severity.
Nevertheless, in a systematic review of 7 studies (only three of which were quantitative), the authors concluded that a favourable effect of oral vitamin D supplementation in patients with psoriasis could not be verified but called for more randomised trials to address this issue. However, the available studies did not consider a seasonal effect since vitamin D is produced in the skin by the action of UVB radiation.
In the present trial, researchers focused on trying to establish whether oral vitamin D provided during the winter months, given to psoriasis patients with low serum levels of the vitamin, would have a beneficial effect on disease severity.
The study recruited adult patients with active plaque psoriasis and 25-hydroxyvitamin D (25[OH]D) levels of less than 24 ng/mL. Cholecalciferol (oral vitamin D) was given at a loading dose of 100 000 IU, followed by 20 000 IU/week or matching placebo, for a period of 4 months.
The primary outcome was the change in the Psoriasis Area Severity Index (PASI) score, which is a measure of disease severity. The researchers also looked at the change in Dermatology Life Quality Index scores.
Oral vitamin D supplementation and psoriasis disease severity
A total of 122 participants with a mean age of 53.6 years (37.7% female) were randomised to either oral supplementation (60) or placebo. The mean baseline PASI score was 3.1.
After 4 months, the mean 25(OH)D level was 29.7 ng/mL and 12.0 in the placebo group. However, while serum levels of vitamin D had increased among participants in the intervention arm, there was no significant difference in the PASI score between the groups (adjusted difference, AD = 0.11, 95% CI -0.23 to 0.45, p = 0.52). In addition, there was no significant difference in DLQI scores between the groups (AD = -0.86, 95% CI -1.9 to 0.19, p = 0.11).
The authors concluded that oral vitamin D supplementation did not affect psoriasis severity and suggested that low baseline severity scores might have accounted for lack of measurable effect.
They also added that since less than half of the intervention group achieved a serum 25(OH)D level of 30 ng/ml, this may have affected the results.
Citation
Jenssen M et al. Effect of Vitamin D Supplementation on Psoriasis Severity in Patients With Lower-Range Serum 25-Hydroxyvitamin D Levels: A Randomized Clinical Trial. JAMA Dermatol 2023