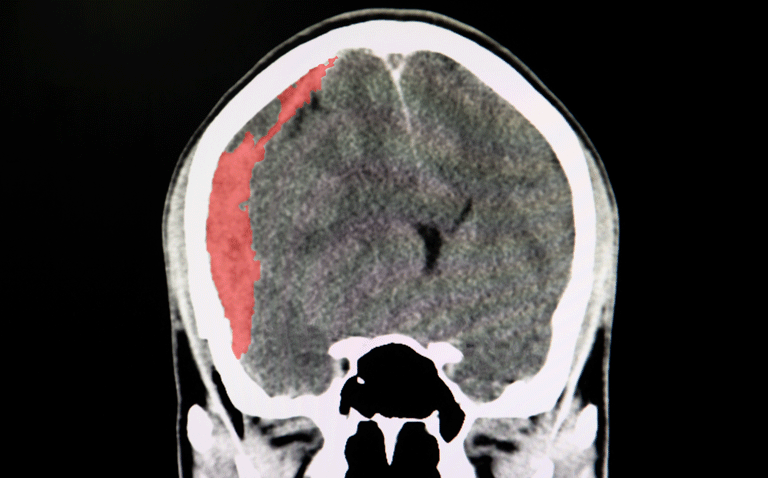
Anticoagulation reversal agents used for intracranial haemorrhage have similar levels of efficacy and safety according to a systematic review
Anticoagulant reversal agents use following an intracranial haemorrhage, all appear to have a similar level of efficacy and safety according to the findings of a meta-analysis by US researchers.
The direct oral anticoagulants (DOACs) are increasingly preferred over warfarin in DOAC-eligible patients with atrial fibrillation and patients with venous thromboembolism. In fact, the more widespread introduction of these agents has been generally well received by patients who report a high level of treatment satisfaction.
Nevertheless, anticoagulant agents are associated with an increased risk of bleeding and the annual rate of intracranial haemorrhage in those taking DOACs is 0.1% to 0.2%. Several anticoagulant reversal agents are currently available and approved. For example, andexanet alfa (AA) has been approved where reversal of anticoagulation is needed due to life-threatening or uncontrolled bleeding with apixaban or rivaroxaban.
Similarly, idarucizumab is approved for the specific reversal of dabigatran. Prothrombin complex concentrates have been developed to contain highly concentrated coagulation factors and one particular agent, 4-factor prothrombin complex concentrate (4F-PCC), has been found to be a good treatment option in patients requiring DOAC reversal.
However, the newer and traditional agents have not been directly compared. As a result, in the present study, the US researchers undertook a systematic review of the safety and efficacy of these non-specific (i.e., 4F-PCC) and targeted anticoagulant reversal agents in patients with DOAC-related intracranial haemorrhage (ICH).
Included studies were those in which patients with an intracranial haemorrhage had been treated with a DOAC, there was reversal of the DOAC and anticoagulant reversal outcomes such as thromboembolism and mortality were reported. The primary outcome was the successful reversal of anticoagulation.
Anticoagulant reversal of DOAC therapy
A total of 36 studies including 1832 patients with an ICH and a mean age of 76 years (57% male) met the inclusion criteria.
For patients treated with 4F-PCC, anticoagulant reversal occurred in 77% of patients, compared to 75% for AA and 82% for idarucizumab when reversing dabigatran.
In terms of safety, all-cause mortality was also broadly similar for 4F-PCC and AA (26% vs 24%) and lower for idarucizumab (11%). Thromboembolic events were similar for 4F-PCC and idarucizumab (8% vs 5%) and slightly higher for AA (14%).
The authors concluded that while there were no direct head-to-head comparisons available, their findings suggested that the overall anticoagulation reversal, mortality, and thromboembolic event rates appeared similar among available DOAC reversal agents for managing ICH.
Citation
Chaudary R et al. Evaluation of Direct Oral Anticoagulant Reversal Agents in Intracranial Hemorrhage: A Systematic Review and Meta-analysis. JAMA Netw Open 2022.