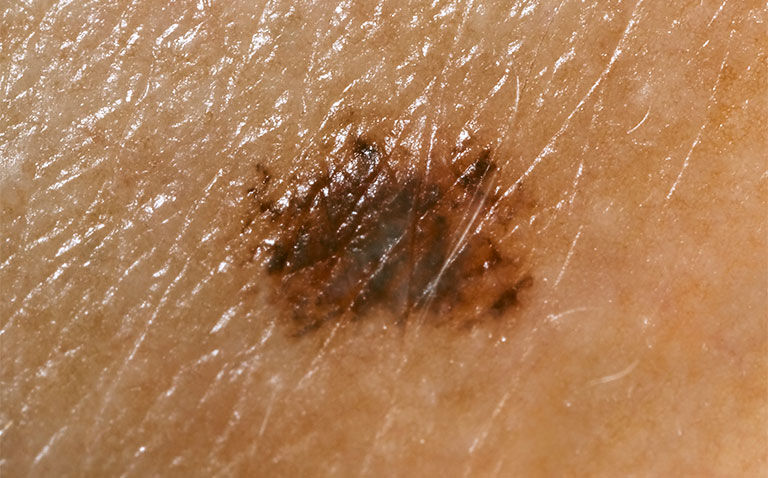
Cases of melanoma in situ are on the rise, but why is this the case and does it pose a greater risk of death among those diagnosed with the cancer? Clinical writer Rod Tucker considers the evidence.
Globally, there were an estimated 325,000 diagnoses of cutaneous melanoma – or simply melanoma – in 2020, with a corresponding 57,000 deaths. Based on current trends, it is estimated that there could be a 68% increase in melanoma-related deaths by 2040, although there are hopes that a melanoma vaccine used in the advanced stages of the disease might reduce these deaths.
Melanoma is now the 17th most common cancer worldwide, with cases steadily rising over the last 40 years. For example, the annual number of melanoma cases in men has increased from 837 per year between 1981 and 1985 to 6,963 per year between 2016 and 2018 – a more than eight-fold increase.
While invasive melanoma cases have increased substantially over the last 30 years, there has been a greater rise in the level of melanoma in situ, also known as a stage 0 melanoma, which are essentially benign lesions. The magnitude of the increase of melanoma in situ was revealed in a 2022 comparative study of invasive and in situ melanoma incidence in three predominately white populations in Australia, the US and Scotland.
The team considered the average annual percentage rate of change (AAPC) for the two types of melanoma and the results were somewhat surprising. While there was a significant increase in the AAPC for invasive melanoma in all three areas between 1982 and 2018, the largest increase was for melanoma in situ. For example, in white US males, the AAPC for invasive melanoma was 2.9 whereas for melanoma in situ, the figure was 8.7. A similar level of increase was seen across all three populations.
The purported culprit for the rise in melanoma cases is increased sun exposure, largely because of UV radiation. But does this really account for the observed increased incidence?
Melanoma in situ and UV radiation
If greater exposure to sunlight believed to be responsible to the higher levels of melanoma, what does the research actually show?
In a meta-analysis of risk factors for melanoma focusing on sun – and therefore UV radiation – exposure, the authors extracted data from 57 studies and provided relative risk (RR) estimates for the different types of sun exposure. For total sun exposure, the risk of melanoma increased by 34% (RR = 1.34) and by 61% for intermittent exposure (RR = 1.61). In addition, there was a much stronger risk in those with a history of sunburn (RR = 2.03).
Yet, even in the worse case scenario, exposure to sunlight leads to no more than a two-fold increase in the risk of melanoma, much less than the actual eight-fold increased alluded to earlier. So what else could account for this discrepancy?
Greater diagnostic scrutiny
One possible reason for the higher incidence of melanoma in situ is that it is merely an artefact of increased skin cancer screening. This, it seems, is a more plausible explanation and there is some evidence to support it.
One study from 2012 suggested that today’s dermatopathologists are more inclined to diagnose melanoma than their predecessors. The study looked at biopsy specimens diagnosed as dysplastic nevi with severe atypia from 20 years earlier. Interestingly, researchers observed a general trend towards the reclassification of severely atypical melanocytic tumours as melanoma by all study participants. As the diagnosis of cutaneous melanocytic lesions relies on a pathologist’s visual assessment of biopsy material, it is ultimately somewhat subjective.
This point was clearly illustrated in a study from 2017 which considered the interpretation of pathologists’ diagnoses of melanocytic skin lesions. When a pathologist was asked to rate the same skin biopsies on two occasions, eight months apart, they demonstrated good reproducibility. However, the intraobserver reproducibility was much lower and, as the authors concluded, ‘diagnoses spanning moderately dysplastic nevi to early stage invasive melanoma were neither reproducible nor accurate.’
Melanoma in situ malignant transformation
If the rise in overall melanoma diagnoses merely reflects an greater detection of melanoma in situ, is this still a cause for concern? To put it another way, to what extent do these benign lesions undergo malignant transformation and thus increase the risk of death?
This was the question addressed in a recent study published in JAMA Dermatology. The researchers examined the mortality risk among those diagnosed with a melanoma in situ. Following 137,872 patients with a first and only diagnosis of melanoma in situ, the researchers observed that 15 years after their diagnosis, the melanoma-specific survival was 98.4%.
Perhaps more interesting was the fact that the 15-year relative survival compared to the general population was 112.4%. In other words, virtually everyone diagnosed with a melanoma in situ was not only still alive 15 years later, but appeared to outlive those without the cancer.
But what if a melanoma in situ becomes invasive? Using a subgroup of 156,251 patients, the researchers observed that the 15-year cumulative incidence of a secondary primary invasive melanoma was 8.9% and 14.1% for a second primary melanoma in situ. Nonetheless, this had little impact on either melanoma or relative 15-year mortality which remained virtually unchanged at 98.2% and 126.7% respectively. Even among those who developed a second melanoma in situ, there was only a small reduction in both the 15-year melanoma and relative survival.
Risk vs benefit of screening
Based on these findings, questions have been raised as to whether it is time to stop skin cancer screening. In fact, this was the subject of a recent study by Australian researchers who tried to estimate the possible risk of over diagnosis of melanoma by the comparing the subsequent melanoma incidence and biopsy rates among people who either did or did not undergo skin screening.
When analysing all melanomas arising within the first year following recruitment, there was a 59% higher risk of a melanoma in situ but not for invasive melanomas. The authors calculated that the absolute risk of developing a melanoma after five years, in those who underwent screening would be 1.94% compared to 1.45% in those who were not screened. This, they said, equates to a number needed to screen to detect one excess melanoma of about 206.
Although this was a theoretical study, real-world data also suggests that failure to screen patients does not increase the risk of missed diagnoses. For example, the interruption of screening due to Covid-19 did not lead to unfavourable primary tumour characteristics of melanoma.
While it might seem prudent to continue screening but only for high risk patients, this is by no means an easy task given how the risk factors for melanoma are multi-factorial and based on both genetic and personal attributes.
With the development of new AI-based technology, it is anticipated that skin cancer screening could become both faster and possibly more targeted. Nevertheless, medico-legal concerns of a missed diagnosis are unlikely to recede in the near future, prompting an increased level of screening.
Perhaps it is time to raise the diagnostic bar for biopsies and avoid the labelling of benign lesions like melanoma in situ, especially given the devastating impact of a cancer diagnosis – even if unwarranted – on a patient’s wellbeing.