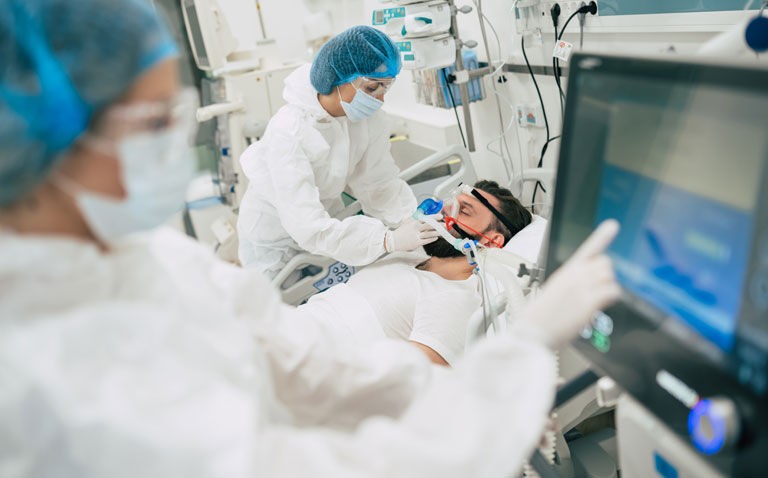
The multi-inflammatory index has been shown to an effective biomarker for the prediction of mortality in critically ill COVID-19 patients
A multi-inflammatory index (MII) biomarker have been shown to have good predictive power for mortality among COVID-19 patients admitted to an intensive care unit (ICU). This was the main finding of a study by a team of Turkish researchers.
It is common among patients with severe COVID-19 to develop acute respiratory distress syndrome (ARDS) which represents a life-threatening form of respiratory failure and after the initial infection, neutrophils, which form part of the innate immune system, rapidly infiltrate the lungs.
However, lymphocytes also have an important role in both immune homeostasis and inflammatory responses throughout the body and lymphopenia has been shown to be an effective and reliable indicator of the severity and hospitalisation in COVID-19 patients.
Nevertheless, infection with COVID-19 produces several biochemical abnormalities including elevation of C-reactive protein in patients with severe disease, together with hyper-inflammation and a cytokine storm. In fact, alterations in the level of several markers has been shown to be of value in predicting the prognosis of patients infected with the virus.
One particular biomarker, the multi-inflammatory index (MMI), which includes the neutrophil to lymphocyte ratio (NLR) and C-reactive protein (CRP), has been shown to have good prognostic mortality value when originally examined in patients with metastatic colorectal cancer undergoing first-line chemotherapy.
As other research has found that both the neutrophil-lymphocyte ratio and C-reactive protein are significantly higher in patients with COVID-19 and who subsequently die, the Turkish team wondered if the MII – which includes both measures – would have prognostic value for identifying which critically ill patients with COVID-19, were at a higher risk of mortality.
The team retrospectively analysed data on COVID-19 patients admitted to an ICU and compared the prognostic value of MII with a range of inflammatory biomarkers including the urea to albumin ratio, CRP to albumin ratio and the D-dimer to albumin ratio.
Multi-inflammatory index and COVID-19 mortality
A total of 348 patients with a median age of 74 years (59% male) were admitted to ICU due to COVID-19 and included in the analysis.
Overall, 24.7% of patients survived and the remainder died. While co-morbidities such as hypertension, diabetes and COPD were numerically higher among those who died, these differences were not statistically different.
Using multiple logistic regression, among all the inflammatory measures used, only MII was found to be an independent predictor of mortality (odds ratio, OR = 0.99, 95% CI 0.99 – 0.99, p = 0.03). Other significant predictors included age (OR = 1.07), the NLR (OR = 1.07).
Commenting on their results, the authors suggested that the likely reason why the NLR ratio was elevated in COVID-19 patients was because of an increased neutrophil count and a corresponding lymphopenia.
They concluded that MII represents a simple and practical biomarker which could help identify COVID-19 patients with a poor prognosis and called for further studies to validate these retrospective findings.
Citation
Gozdas HT et al. Multi-inflammatory Index as a Novel Mortality Predictor in Critically Ill COVID-19 Patients J Intensive Care Med 2022