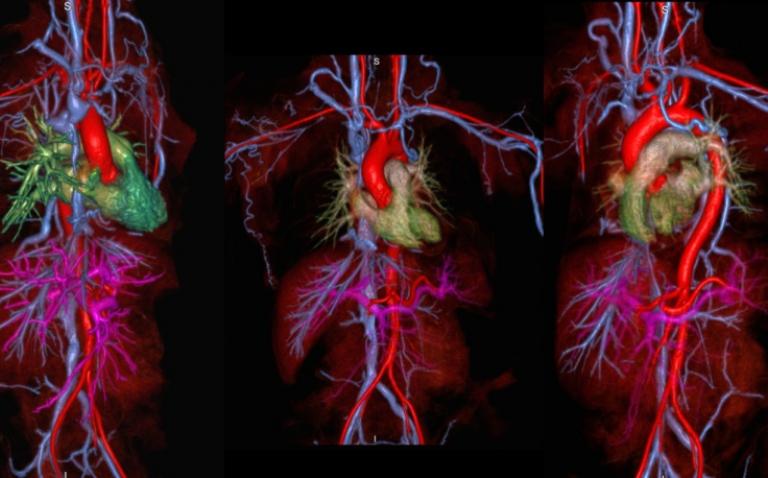
Magnetic resonance angiography (MRA) is a magnetic resonance imaging (MRI) exam that takes pictures of the blood vessels. Physicians use the images to diagnose diseases of the blood vessels, such as aneurysms or blockages.
During the test patients lie on a table inside a tunnel-like tube and must remain still. A dye, called a contrast agent, is injected into the veins so the vessels can be seen more clearly. Patients are given a headset to block out noise from the scanner. An MRA can typically take 30 minutes to one hour, from start to finish.
“Lengthy scans can be problematic for patients with even modest levels of claustrophobia who may refuse the test or ask for it to be stopped early,” said Dr Puja Shahrouki, research fellow, David Geffen School of Medicine at UCLA, Los Angeles, US. “They also limit the number of patients that can be scanned each day. In addition, the usual gadolinium-based contrast agents can be an issue for patients with kidney problems.”
This study aimed to shorten the scan time and still produce high quality images. The researchers used ferumoxytol as the contrast agent as it stays within the vascular system for much longer than gadolinium-based dyes. With gadolinium-based agents, there is a short time when the images can be taken, which means patients have to wait in the scanner while the clinician watches the dye move through the body in order to capture the images when the dye enters the blood vessels.
The UCLA study included seven claustrophobic patients aged 11 to 63 years with kidney failure. There were four men and three women. All patients said they were reluctant to undergo MRA due to claustrophobia, but agreed to a trial of up to ten minutes in the scanner bore.1
Eight MRA scans using ferumoxytol were conducted. All scans were completed and there were no adverse events. Scans took an average of 6.27 minutes (range four to ten minutes). All scans were high quality and allowed full visualisation of the arterial and venous anatomy from the neck to the thighs.
“Despite being claustrophobic, all patients completed the MRA and the images could be used for diagnosis of the entire vascular system,” said Dr Shahrouki. “Some of the scans were done in less than five minutes once the procedure started, making it much shorter than the tests currently used in medical practice.”
The researchers have shown that the test can be used to diagnose venous and arterial diseases, such as central venous occlusion and aneurysms, and to aid preprocedural planning, for example in transcatheter aortic valve replacement. In principle, it is possible to scan several patients in an hour as opposed to just one or two, raising promising possibilities for workflow and efficiency.
Dr Shahrouki said: “This method could enable claustrophobic patients to receive lifesaving diagnoses and procedures. For appropriate types of studies, it could also shorten waiting lists and improve the cost-benefit ratio for hospitals.”
The new protocol should be technically easier than current practice because there is no time pressure for taking images. Ferumoxytol is increasingly recognised as an alternate contrast agent in patients with poor kidney function, but is not marketed outside the US. It is approved by the US Food and Drug Administration (FDA) only for the treatment of iron deficiency anaemia in adults with chronic kidney disease.
Hypersensitivity reactions have occurred in patients receiving ferumoxytol as a high dose for therapy in a short period of time, and the FDA has warned against this. The new MRA protocol administers the dye by slow infusion outside the MRI machine while monitoring the patient’s vital signs, in compliance with FDA guidelines. A preliminary study showed this was safe1 and a larger registry is generating a safety profile of slow infusion under close monitoring. More safety data will be needed before any conclusions can be drawn about the true rate of hypersensitivity reactions and in the meantime close monitoring is the rule.
Dr Shahrouki said: “The protocol could have huge implications for claustrophobic patients and efficient use of scanners. We envisage it being used very widely in patients with a clear clinical indication.”
Photo credit: Dr Paul Finn
References
- The abstract ‘Focused, Whole Body Vascular MR Imaging in Less than Five Minutes with Ferumoxytol’ was presented during Poster Session 3 on 3 February 2018 at 10:15 to 11:00 CET.
- Nguyen KL, Yoshida T, Han F, Ayad I, Reemtsen BL, Salusky IB, Satou GM, Hu P, Finn JP. MRI with ferumoxytol: A single center experience of safety across the age spectrum. J Magn Reson Imaging. 2017;45(3):804–812. doi: 10.1002/jmri.25412